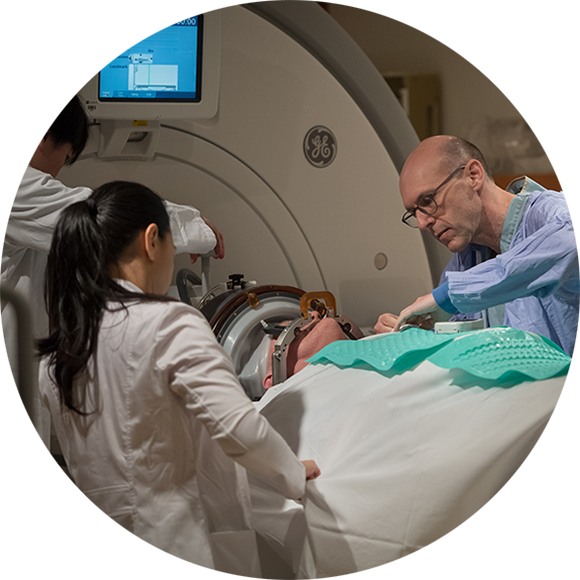
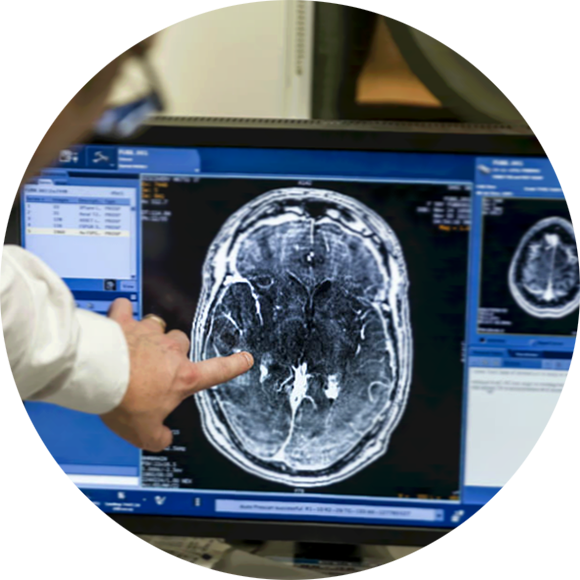
Focused ultrasound
Focused ultrasound (FUS) is a non-invasive, image-guided surgical technology that uses ultrasound energy to target specific areas of the brain and body in the treatment, or investigation of safety and efficacy in a number of indications including; essential tremor, brain cancer, Alzheimer’s disease, severe depression, and Parkinson’s disease. It is considered to be scalpel-free, avoiding incisions to the skin. Sunnybrook is a global leader in FUS research and clinical trials, and the first Centre in Canada to be recognized as a Centre of Excellence in Focused Ultrasound.
Timeline of accomplishments in focused ultrasound
View some of our research accomplishments in timeline below, organized in reverse chronology.
Click through the dates in the timeline below to view more photos and milestones
-
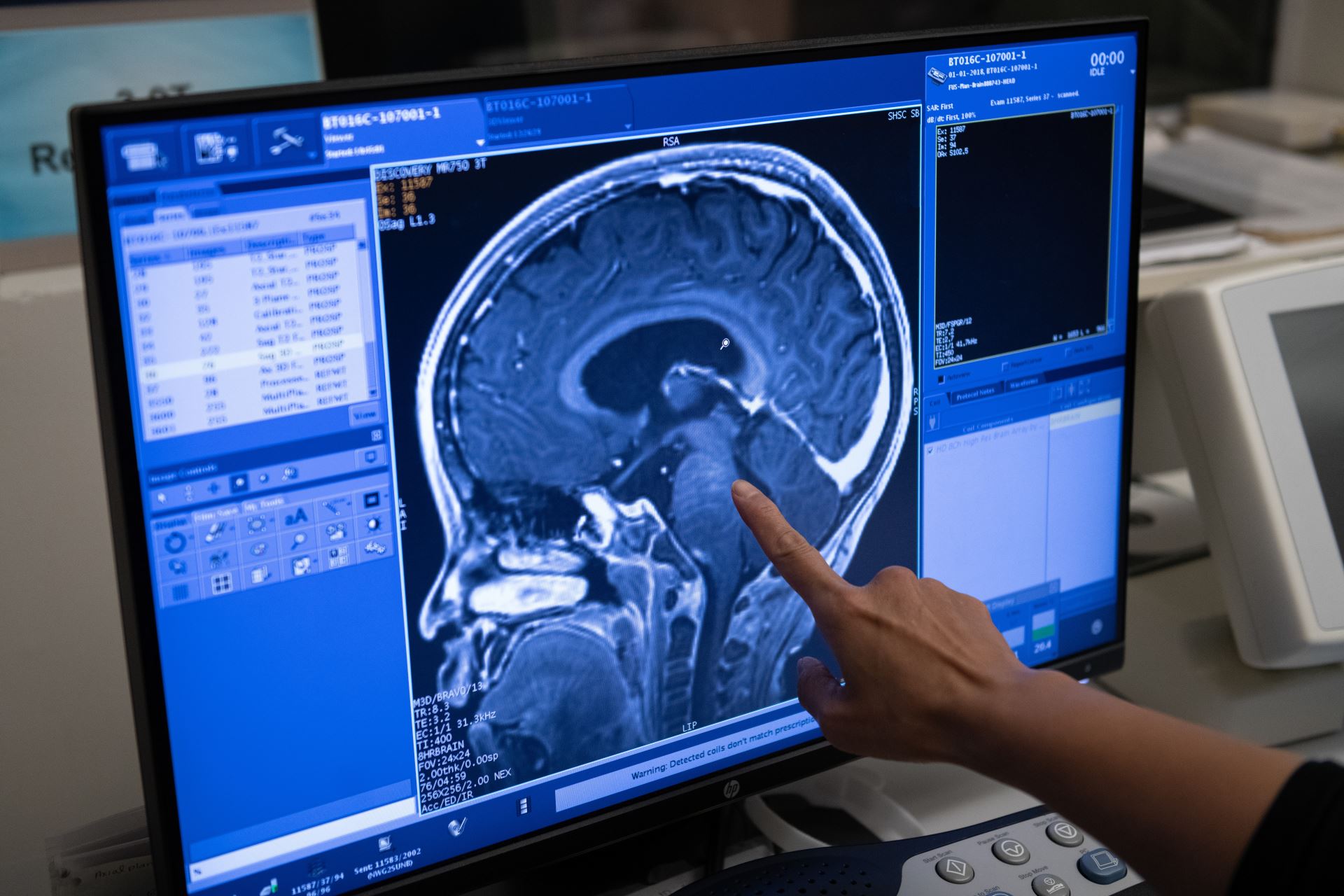
Diffuse Intrinsic Pontine Glioma
Jan 2023 - World first: Researchers and physicians at Sunnybrook Health Sciences Centre and The Hospital for Sick Children (SickKids) are the first in the world to use MRI-guided focused ultrasound to open the blood-brain barrier and deliver chemotherapy in Diffuse Intrinsic Pontine Glioma (DIPG), an aggressive and terminal pediatric brain tumour. Learn more.
 Click through the dates in the timeline above to view more photos and milestones
Click through the dates in the timeline above to view more photos and milestones -
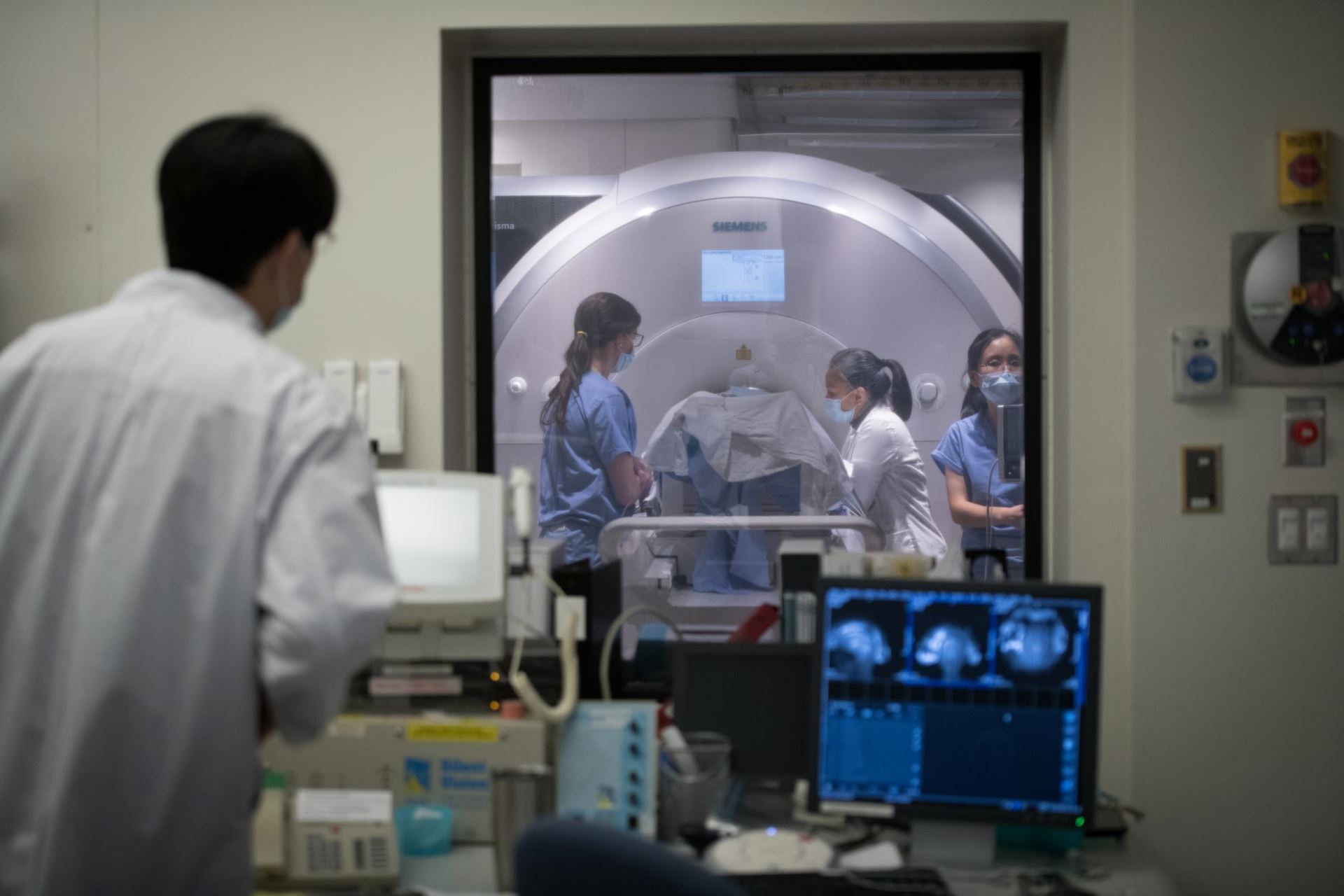
Parkinson’s Disease
Sept 2022 - World first study finding: focused ultrasound for delivery of direct-to-brain therapeutics in Parkinson’s disease is safe. Learn more.
 Click through the dates in the timeline above to view more photos and milestones
Click through the dates in the timeline above to view more photos and milestones -
Marking a 10-year milestone
May 2022 - Sunnybrook's leading edge research in focused ultrasound for the brain and how it will revolutionize treatment in the future. Learn more.
 Click through the dates in the timeline above to view more photos and milestones
Click through the dates in the timeline above to view more photos and milestones -
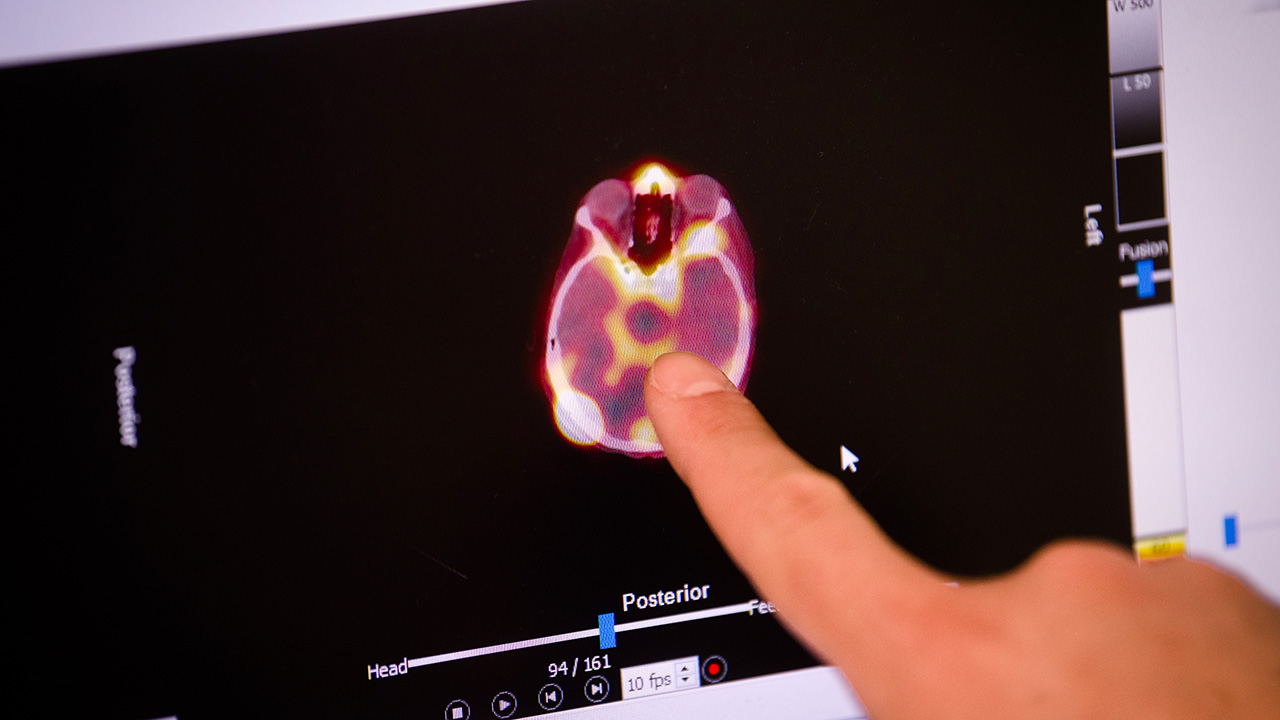
Breast Cancer Brain Metastases
October 2021 - Researchers at Sunnybrook Health Sciences Centre capture world-first images of the safe delivery of an antibody therapy drug to tumours which spread to the brain from breast cancer, across the blood-brain barrier using MRI-guided focused ultrasound. Learn more.
 Click through the dates in the timeline above to view more photos and milestones
Click through the dates in the timeline above to view more photos and milestones -
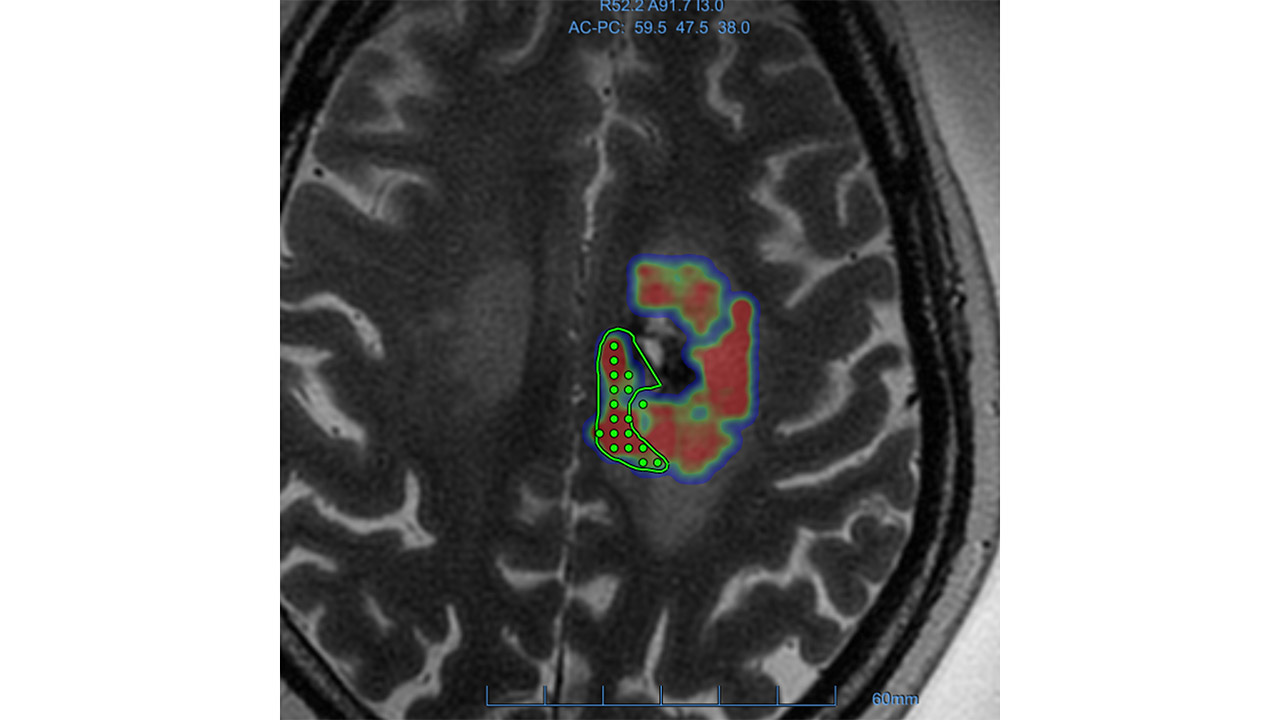
Focused Ultrasound and Liquid Biopsy
March 2021 - In a first-ever study, Sunnybrook researchers have demonstrated that MRI-guided focused ultrasound technology can improve the detection of brain cancer biomarkers with the temporary opening of the blood-brain barrier to aid liquid biopsy, also known as virtual biopsy. Learn more.
-
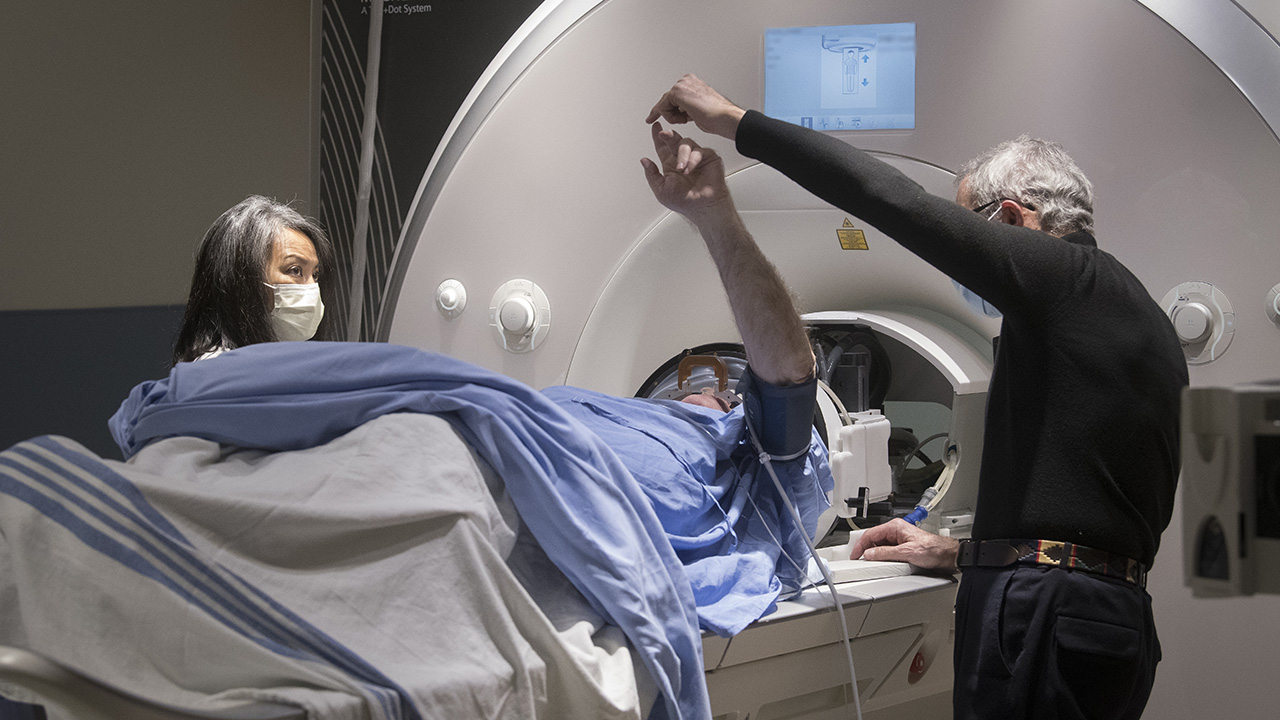
Bilateral Essential Tremor
November 2020 - Sunnybrook researchers launch a clinical trial for focused ultrasound in bilateral essential tremor. Learn more.
 Click through the dates in the timeline above to view more photos and milestones
Click through the dates in the timeline above to view more photos and milestones -
Parkinson's Disease
October 2020 - World first: focused ultrasound opens blood-brain barrier for delivery of therapeutic in Parkinson's disease. Learn more about this research.
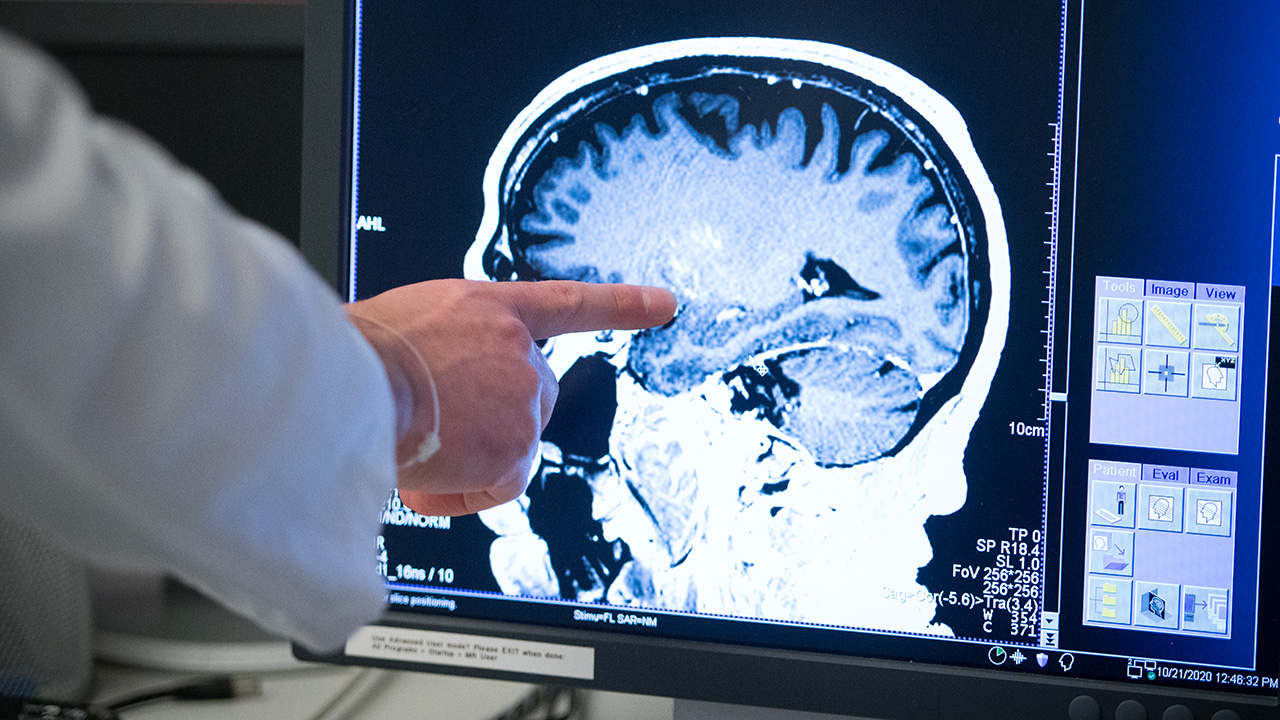 Click through the dates in the timeline above to view more photos and milestones
Click through the dates in the timeline above to view more photos and milestones -
Breast Cancer Brain Metastases
November 2019 - Canadian first: First patient with breast cancer that has spread to the brain treated with focused ultrasound and Herceptin. Learn more about this research and read the first patient's story.
 Click through the dates in the timeline above to view more photos and milestones
Click through the dates in the timeline above to view more photos and milestones -
Alzheimer's Disease
January 2019 - World first: Blood-brain barrier opened in multiple regions in a patient with Alzheimer’s disease. Learn more.
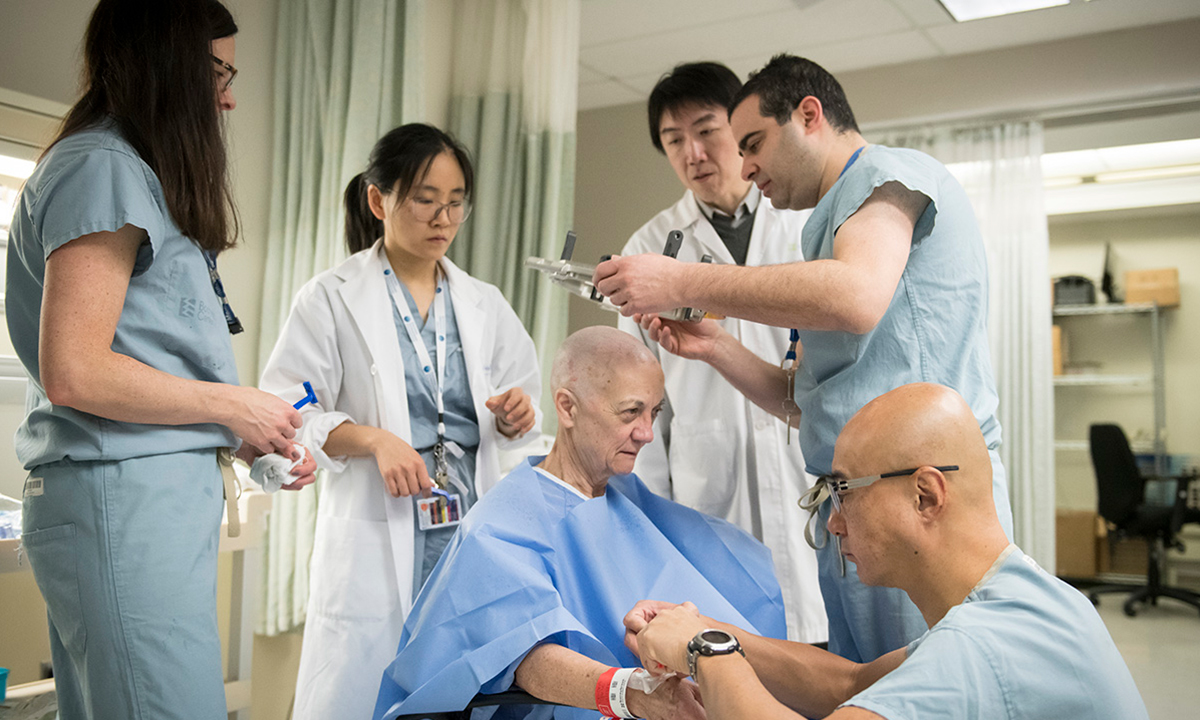 Click through the dates in the timeline above to view more photos and milestones
Click through the dates in the timeline above to view more photos and milestones -
Glioblastoma
November 2018 - Phase 2 trial using focused ultrasound to open the blood-brain barrier in a patient with glioblastoma (GBM). Goal is to enhance the delivery of chemotherapy to GBM. Learn more.
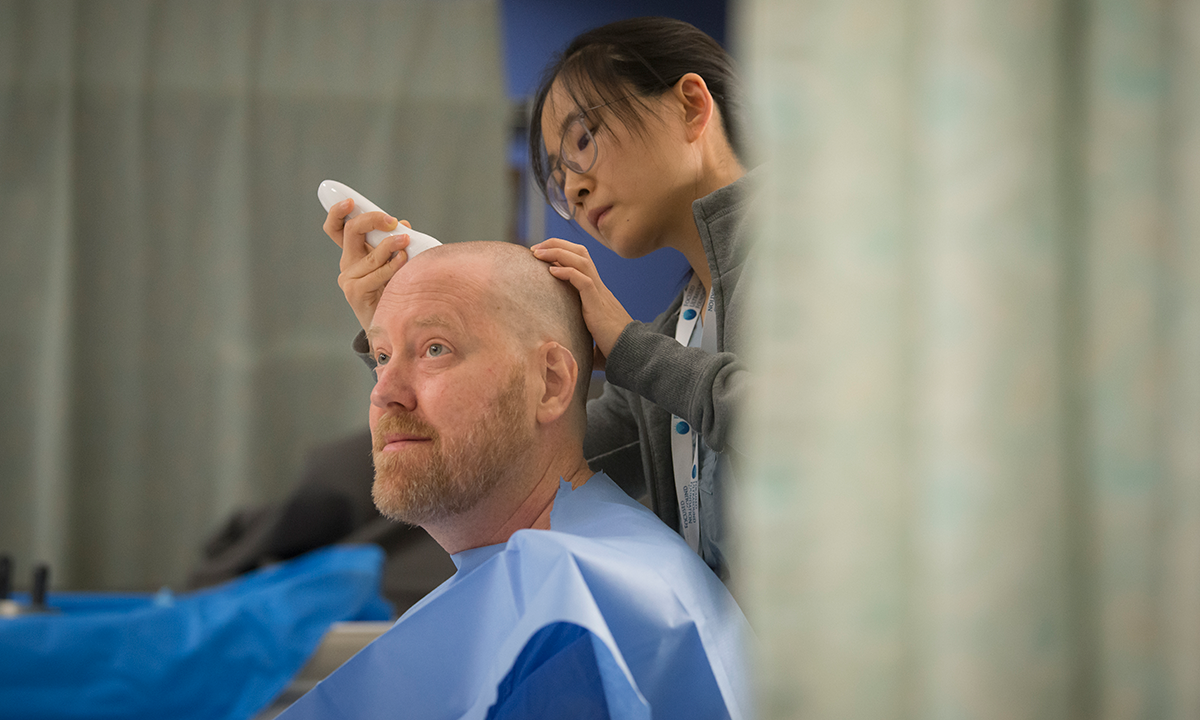 Click through the dates in the timeline above to view more photos and milestones
Click through the dates in the timeline above to view more photos and milestones -
100th essential tremor patient treated
August 2018 - 100th Sunnybrook patient is treated for essential tremor with focused ultrasound since our researchers revolutionized this non-invasive world first procedure in 2012. Learn more.
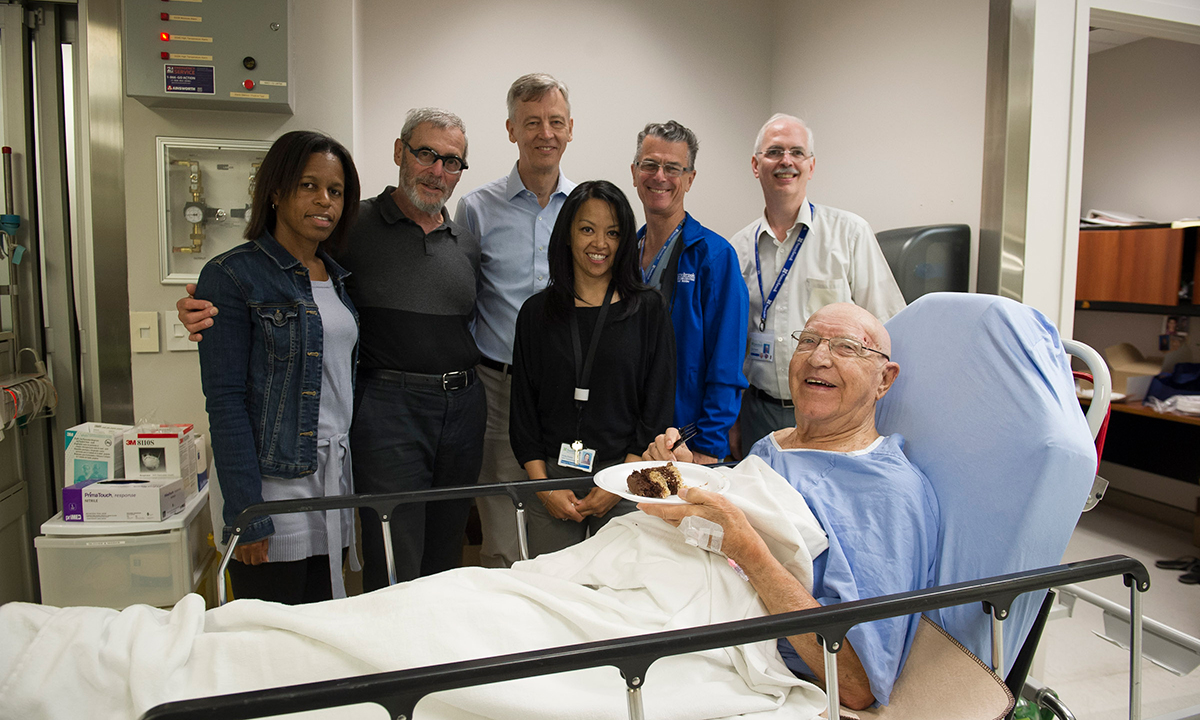 Click through the dates in the timeline above to view more photos and milestones
Click through the dates in the timeline above to view more photos and milestones -
Major depression
May 2018 - North American first trial to investigate the safety and effectiveness of FUS for patients with major depression. Learn more.
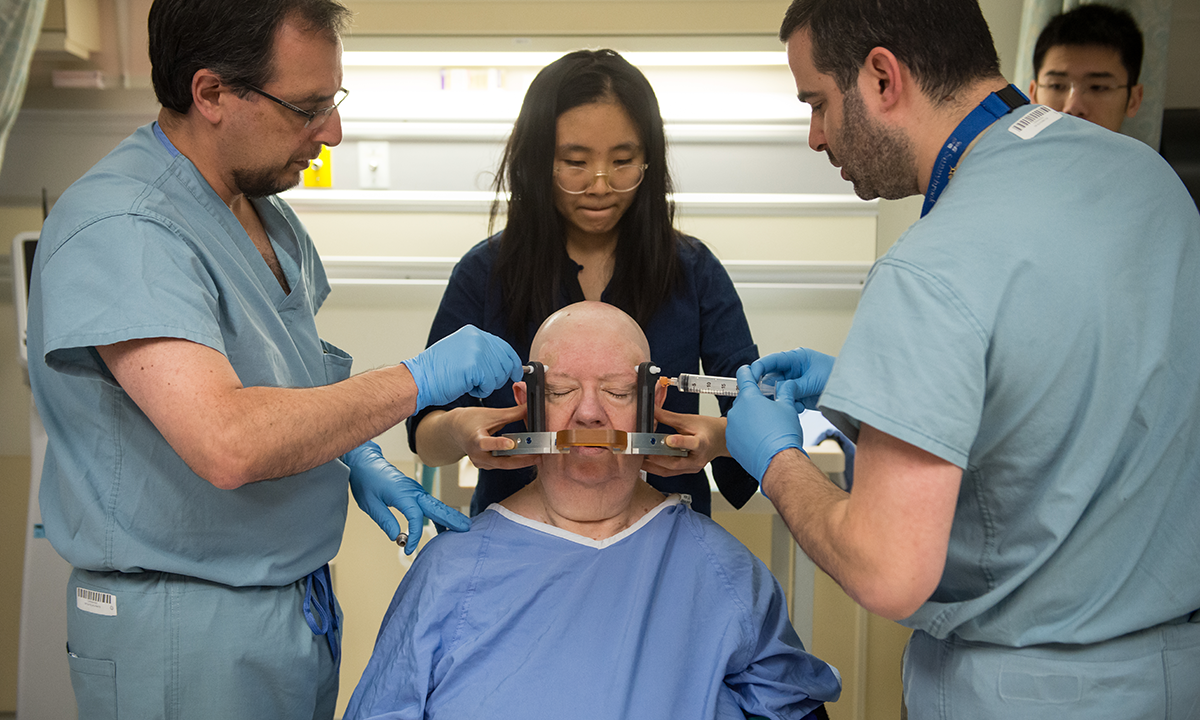 Click through the dates in the timeline above to view more photos and milestones
Click through the dates in the timeline above to view more photos and milestones -
ALS
April 2018 - World first: Sunnybrook researchers begin a study investigating the safety and feasibility of using MRI-guided focused ultrasound to open the blood-brain barrier of the motor cortex in patients with ALS. Sunnybrook is the only centre pursuing this kind of work with ALS patients. Learn more.
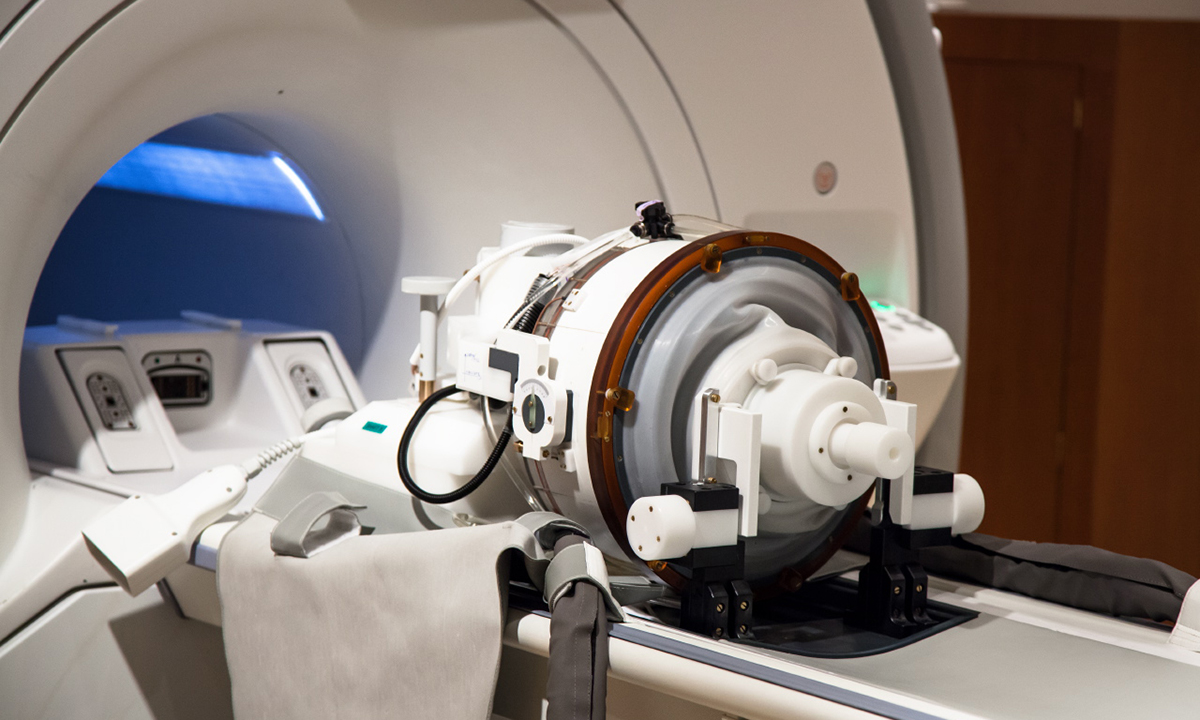 Click through the dates in the timeline above to view more photos and milestones
Click through the dates in the timeline above to view more photos and milestones -
Obsessive-Compulsive Disorder (OCD)
July 2017 - North American first trial exploring the safety of focused ultrasound for treatment-resistant OCD. Learn more about the clinical trial and read the first patient’s story.
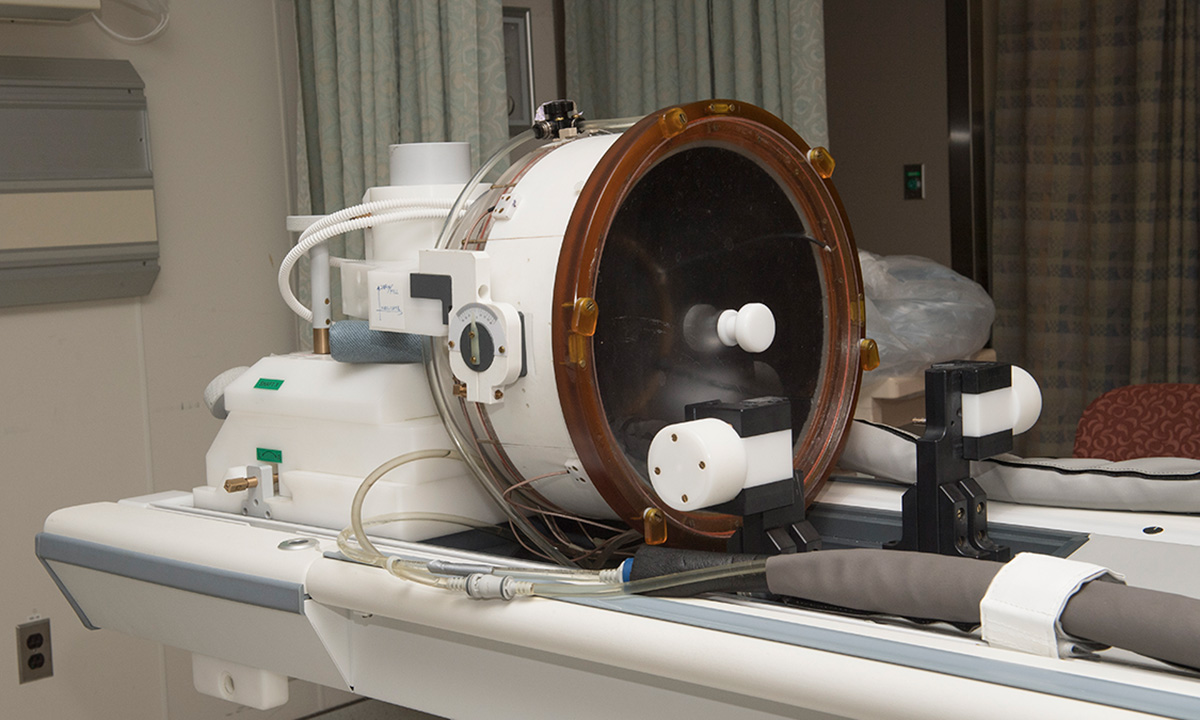 Click through the dates in the timeline above to view more photos and milestones
Click through the dates in the timeline above to view more photos and milestones -
Alzheimer's disease
May 2017 - Sunnybrook researchers made history launching the world’s first clinical trial to evaluate the safety and feasibility of using focused ultrasound to open the blood-brain barrier in people with Alzheimer’s disease. Learn more.
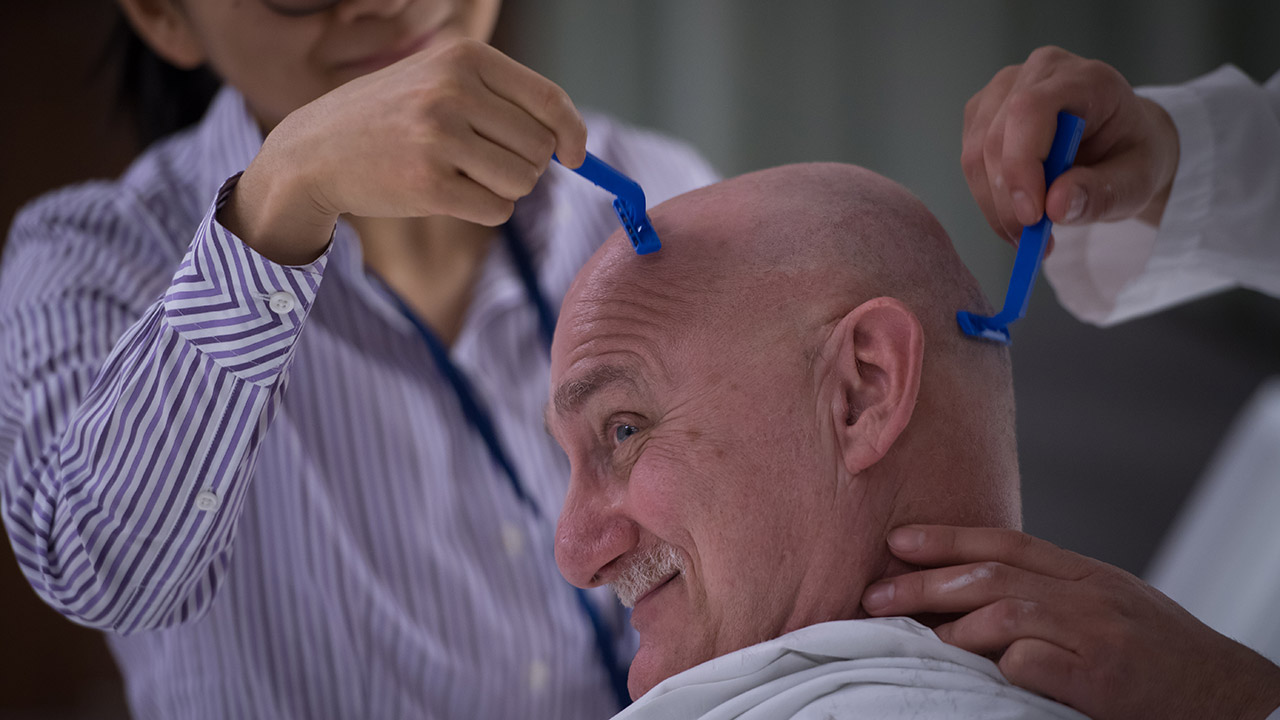 Click through the dates in the timeline above to view more photos and milestones
Click through the dates in the timeline above to view more photos and milestones -
Essential tremor
August 2016 - Scalpel free surgery for essential tremor is effective and safe. Learn more.
 Click through the dates in the timeline above to view more photos and milestones
Click through the dates in the timeline above to view more photos and milestones -
Brain tumours
November 2015 - World first blood brain barrier opened non-invasively to deliver chemotherapy. Learn more.
 Click through the dates in the timeline above to view more photos and milestones
Click through the dates in the timeline above to view more photos and milestones -
Essential tremor
In 2012, World First: Sunnybrook researchers conducted the first Canadian trial and only Canadian site in the first international randomized trial for FUS in essential tremor. Four years later scalpel free surgery for essential tremor is determined to be effective and safe.
Click through the dates in the timeline above to view more photos and milestones