Features
Messages
Digest
Short Stories
Over the Threshold
Doctors (and the rest of us) know that the bigger the burn, the worse the outcome. Beyond what precise point, however, are patients most at risk of no return?
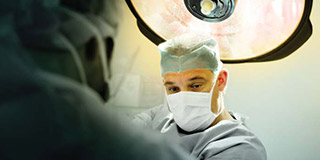
Dr. Marc Jeschke operates on a patient at the Ross Tilley Burn Centre. Jeschke studies cell survival and organ function in severely burned patients at Sunnybrook Research Institute.
Photo: Curtis Lantinga
Over the last 10 years, there have been advances in burn care, mainly stemming from research developments in surgical grafting, wound care and new drugs. As a result, survival rates for burn patients have improved dramatically. Burn care studies published in the 1990s suggest that a burn covering 40% or more of the body results in higher rates of death and serious complications, and thus requires specialist intervention; however, there have been no recent studies quantifying burn size and outcome in light of progress in care.
Dr. Marc Jeschke, a surgeon and scientist in the Trauma, Emergency & Critical Care Research Program at Sunnybrook Research Institute, and colleagues aimed to fill that gap. They did a study to quantify at what point burn size is associated with a higher risk of severe illness and death in children, and thus at what point expert care is required. Results were clear.
“For anyone who sees a child with a burn that is 60% or more, the alarm bell needs to go on,” says Jeschke.
Over this value, they found a higher risk of multi-organ failure, wound sepsis (toxic bacteria), infection and death—all of which point to the need for expert care, he says.
“A child should not even be attempted to be treated in some other burn centre that is not experienced. Children have to be sent as soon as possible to a specialized burn centre, because these patients are at high risk for complications,” says Jeschke, who also directs the Ross Tilley Burn Centre at Sunnybrook and is an associate professor of surgery at the University of Toronto.
The researchers looked at 952 children with burns covering at least 30% of their bodies who were treated at Shriners Hospitals for Children in Galveston, Texas. Patients were categorized by burn size into groups of 10% increments, from 30% to 100% of their bodies; most had burns covering 40% to 50%. Results were published in The Lancet in 2012.
Jeschke and colleagues also correlated outcomes with biochemical markers, and found the presence and concentration of biomarkers in organ function, metabolism and inflammation differed widely in children with a burn size above or below the threshold.
Using biochemical markers confirmed that molecules changed according to burn size, and helped explain survival rates. They also monitored vital signs in liver and kidney function. The study showed that the rate of death was nearly equal in patients with burns covering up to 60% of their bodies, but patients with larger burns were at a much higher risk of dying.
“The beauty of this data is that we not only had demographic data, but we also had biochemical and other markers. That makes the study unique, because we have biochemical approaches backing up the clinical data,” says Jeschke.
He says the results of the study can be applied to all burn patients and will enable burn surgeons to identify patients at high risk for poor outcomes and treat them accordingly.
Next, Jeschke will recruit about 1,000 adult burn patients for a similar study at Sunnybrook that will link clinical and biochemical data. For now, though, the message clinically is simple. “Coming to a specialized burn centre is needed; otherwise, patients will not survive,” he says.
— Eleni Kanavas
Jeschke’s research was funded by the Canada Foundation for Innovation, Institute for Translational Sciences, National Institutes of Health, National Institute on Disability and Rehabilitation Research, Ontario Ministry of Economic Development and Innovation, Physicians’ Services Incorporated Foundation and Shriners Hospitals for Children.
- << Short Stories |
- Previous: Walk This Way •
- Next: How Fractures Heal
- |Connections >>



