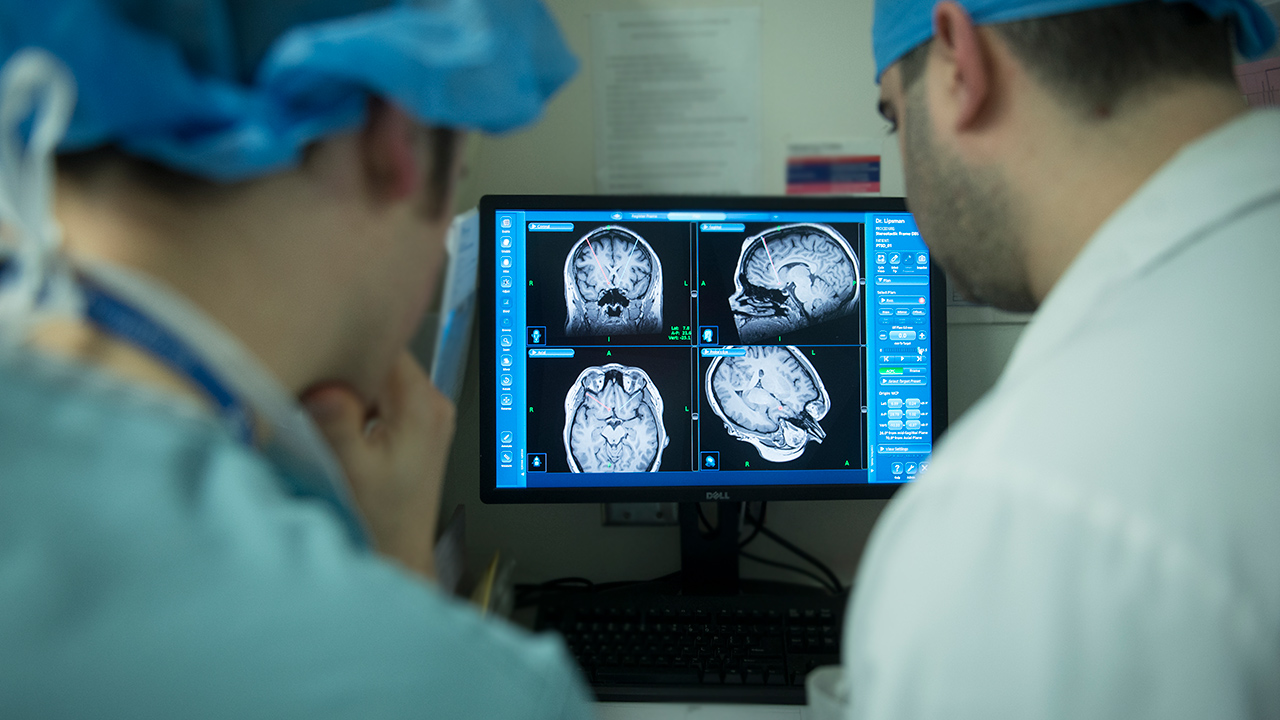
First patient in Canada with treatment-resistant PTSD treated with deep brain stimulation
Sunnybrook researchers are the first in Canada to investigate the use of deep brain stimulation (DBS) to help patients with treatment-resistant post-traumatic stress disorder (PTSD).
PTSD is psychiatric disorder that impacts the lives of more than 3 million Canadians. It can occur after traumatic events such as abuse, natural or unnatural disasters, accidents or military combat. Symptoms may include depression, anxiety, flashbacks and nightmares.
“PTSD is a debilitating mental illness,” says Dr. Peter Giacobbe, study co-principal investigator, psychiatrist and clinical lead at the Harquail Centre for Neuromodulation at Sunnybrook Health Sciences Centre. “Approximately 20 to 30 percent of PTSD patients are considered to have treatment-resistant PTSD because they do not respond to psychotherapy and medication. We need to look at new approaches to treating this group of PTSD sufferers.”
Update - June 2019:
See how Serena Kelly is doing, four months later »
Read more
Neuromodulation is a rapidly evolving field that focuses on the ability to influence brain circuitry. DBS uses implanted electrodes and electrical stimulation to stimulate abnormal activity in areas of the brain. DBS is currently being used in the treatment of symptoms in movement disorders like Parkinson’s disease. In psychiatry, its effectiveness is being investigated for treatment-resistant forms of obsessive-compulsive disorder (OCD) and major depressive disorder (MDD).
“This is the first trial of its kind, dedicated to comprehensively investigating DBS in treatment-resistant PTSD,” says Dr. Nir Lipsman, principal investigator and director at Sunnybrook’s Harquail Centre for Neuromodulation. “We are applying the latest in imaging and technology to develop a 'precision-strike' treatment for PTSD, and determine what influence brain stimulation has on the circuits driving the illness.”
Serena Kelly has lived with the debilitating effects of PTSD for decades, having survived abuse, trauma and personal loss. She tried other forms of treatment, but none were effective in relieving her symptoms. “Living with PTSD is like living in a constant state of fear and always feeling like something bad is going to happen. Like there is danger around every corner. I do hope this does work, not just for me but for others, to give them hope.”
Study investigator Dr. Clement Hamani says, the main objective of this trial is to determine the safety and feasibility of using this leading-edge approach to treatment. “We are investigating next generation treatments for patients with PTSD.”
In 2018, Sunnybrook researchers received a $1.25 million funding grant through the Government of Canada’s Veteran and Family Well-Being Fund to investigate innovative treatments for PTSD and support the first dedicated neuromodulation program for PTSD in Canada at the Harquail Centre for Neuromodulation at Sunnybrook.
This phase I trial will involve five patients, aged 18-70, diagnosed with treatment-resistant PTSD.
For more information or to inquire about eligibility for the trial, please contact Sachie Sharma at harquailcentre@sunnybrook.ca.
Media contact:
Jennifer Palisoc
Sunnybrook Health Sciences Centre
416-480-4040
jennifer.palisoc@sunnybrook.ca
Sunnybrook Health Sciences Centre (Toronto, Ontario) - Inventing the Future of Health Care