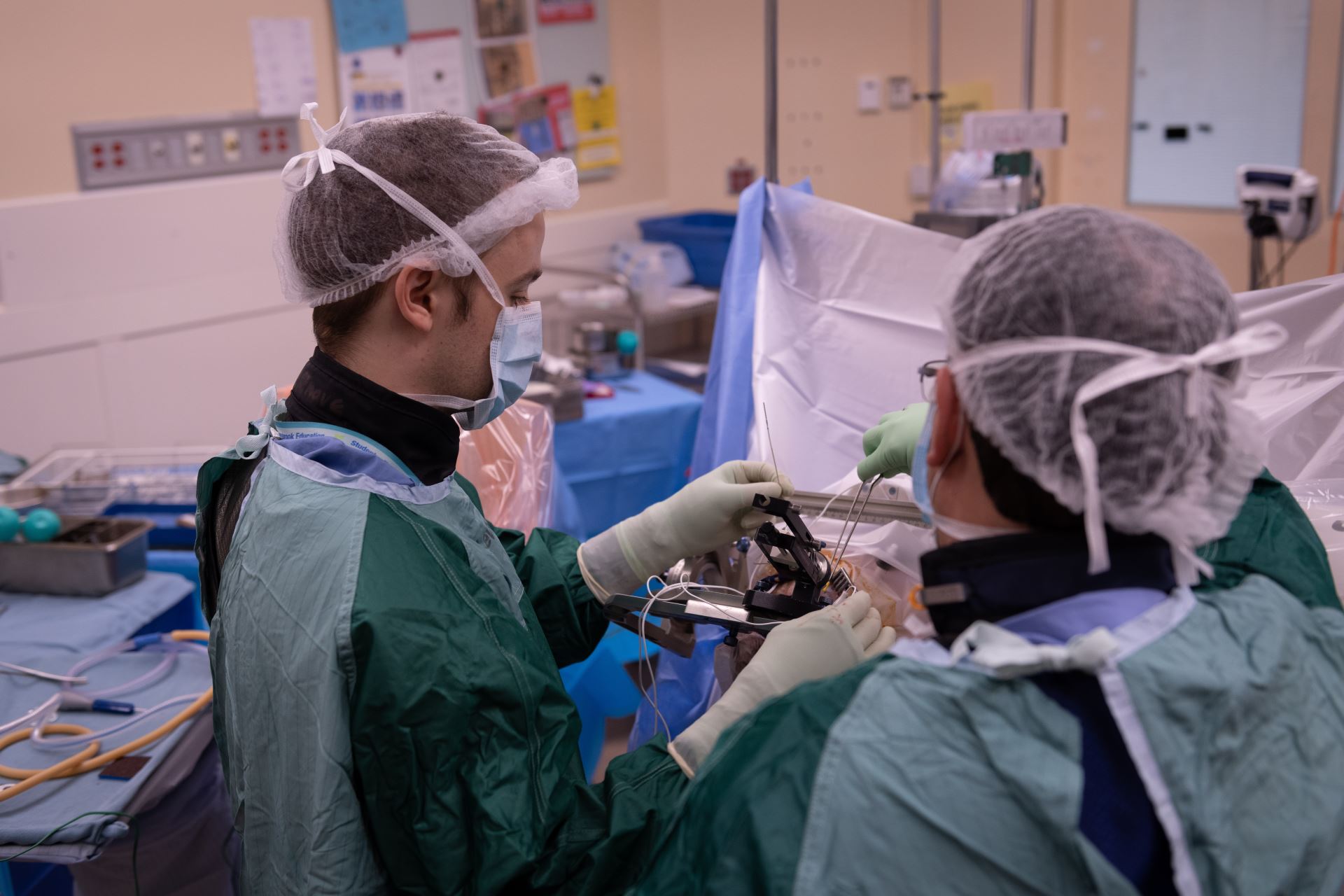
How a Canadian-first study in deep brain stimulation in depression could lead to personalized treatment in the future
In a new leading-edge clinical study, researchers at Sunnybrook Health Sciences Centre are using specialized electrodes in deep brain stimulation to track brain signals in severe depression. The safety trial will also explore whether patient-specific brain ‘signatures’ for mood can be generated, which could help enhance future treatments.
Severe or treatment-resistant depression occurs when a patient has tried psychotherapy, medication, or other methods to alleviate symptoms of depression, but conventional treatments have not helped provide any, or a lasting, improvement.
Dr. Nir Lipsman, neurosurgeon and director of Sunnybrook’s Harquail Centre for Neuromodulation, says this is the first time in Canada that the unique electrode is being used in deep brain stimulation for major depression and explains how this research could lead to a more personalized treatment for patients living with treatment-resistant depression.
What is deep brain stimulation (DBS)?
Dr. Lipsman: Deep brain stimulation, or DBS, is a type of brain surgery, that directly targets brain circuits that aren’t functioning properly in various brain disorders. It is an established procedure around the world for patients with Parkinson’s disease and essential tremor, and currently being investigated for obsessive-compulsive disorder and depression.
In DBS, electrodes are positioned precisely in key brain targets that are responsible for generating and maintaining hard-to-treat symptoms. A pacemaker-like device, which is implanted in the chest, sends electric impulses to the electrodes to stimulate these regions, regulate their activity, and influence symptoms.
How could DBS help to treat depression?
Dr. Lipsman: Over the last 15 years, researchers in Toronto and around the world began exploring conditions where deep brain stimulation could potentially help improve symptoms, such as treatment-resistant depression and post-traumatic stress disorder (PTSD). The idea was if you could use DBS to treat motor circuit conditions, you may be able to use the procedure to treat other circuit-based conditions, such as mood and anxiety disorders.
Our team at Sunnybrook recently published a study that demonstrated deep brain stimulation is safe and potentially effective in treating severe PTSD.
In our current DBS study in major depression, we are specifically targeting regions that we know are involved in depression. The idea is that the constant current or stimulation from a new generation of DBS battery can influence circuits in the brain that are important for depressed mood in an effort to try and reduce the impact of those symptoms and help identify neural signatures for depression.
What is unique about this study?
Dr. Lipsman: In our clinical safety trial, we are specifically looking at a specialized kind of electrode and battery that can both stimulate the brain and record activity at the same time.
The goal is to determine if we can detect a signal that is unique for mood disorders in our patients to better personalize DBS treatment. This is one of the first times in the world and first time in Canada that we’re using these electrodes specifically for patients with depression.
After receiving DBS, study participants will follow their mood closely and every time they feel an acute episode of sadness, for example, or something really triggering for them, they can use an app connected to their pacemaker to record brain activity during that time.
We are then able to download that information, analyze it, and investigate if we can link our patient’s specific brain ‘signature’ to the way they were subjectively feeling. Can we find a signal, some sort of a ‘signature’ related to their mood?
How could finding a brain ‘signature’ help patients living with depression?
Dr. Lipsman: We know these ‘signatures’ exist for symptoms of essential tremor and Parkinson’s disease, but we don’t know yet if they exist in depression. Finding them could lead to the ability to better program brain stimulation so that we can treat patients only when that signature is present. This allows us to potentially tailor stimulation to specific patients and how they feel throughout the course of the day. It’s exciting research where we can, not only learn more about the brain and mood disorders, but potentially enhance treatment for patients in the future.
Learn more about deep brain stimulation at Sunnybrook and how to participate in a study: sunnybrook.ca/dbs
If you need help in an emergency, please call 911 or visit your local emergency department. If you’re feeling like you’re in crisis or need somebody to talk to, please know that help is also available through community resources:
- Find a local crisis resource at sunnybrook.ca/gethelp
- Crisis Services Canada
- Phone: 24-hour, toll-free 1-833-456-4566
- Text: 45645 (4:00 p.m. – midnight Eastern Time)
- Kids Help Phone
- Phone: 24-hour, toll-free, 1-800-668-6868
- Text: 686868 (24 hours, 7 days a week)